Translate this page into:
Asymmetric periflexural exanthema in an adult: A case report
*Corresponding author: Dr. Betsy Ambooken, Department of Dermatology and Venereology, Government Medical College, Thrissur, Kerala, India. joebetsy123@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Ambooken B, Davul H, Muhammed K. Asymmetric periflexural exanthema in an adult: A case report. J Skin Sex Transm Dis 2019;1:35-7.
Sir,
Asymmetric periflexural exanthema (APE) or unilateral laterothoracic syndrome is a morbilliform eczematous and self-limiting cutaneous reaction noted in children during winter and spring.[1] It derives its name as the eruptions usually begin on one side of the body in majority of cases (75%). Although the lesions may subsequently spread to the other side within 1–2 weeks, the asymmetrical nature is maintained throughout the illness. This disease predominantly affects children, with very few documented reports in adults.[2-4] We hereby report a female patient who came to us with diffuse erythematous macular rash mainly affecting the left hemithorax which was diagnosed as APE.
A 33-year-old woman attended our outpatient department with pruritic erythematous eruption of 4 days’ duration. The rash appeared initially near the left axilla which then spread centrifugally to involve the ipsilateral chest and upper limb up to the wrist and back of trunk. She gave a history of a prodromal illness (intermittent low-grade fever, dry cough, and rhinorrhea) one week before the onset of eruption. None of her close contacts or family members had similar illness. The patient denied any history of drug intake or contact with any chemicals or topical preparations prior to the onset of the rash.
Examination revealed a diffuse erythematous macular rash involving the left hemithorax mainly the left side of the upper back, shoulder, the front of the upper chest, and extensor aspect of the upper arm characteristically sparing the pressure points due to the strap of the undergarments [Figure 1].
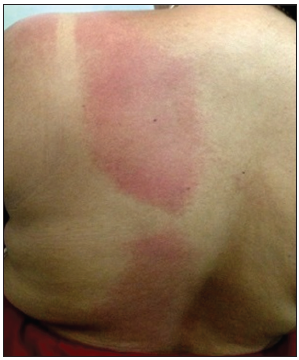
- Diffuse erythematous rash involving the left half of the back of trunk with characteristic sparing beneath the strap of undergarments.
The exanthem also involved the ipsilateral cheek, forearm, and sacral region. Few spillover lesions were present on the right side of the chest [Figure 2].
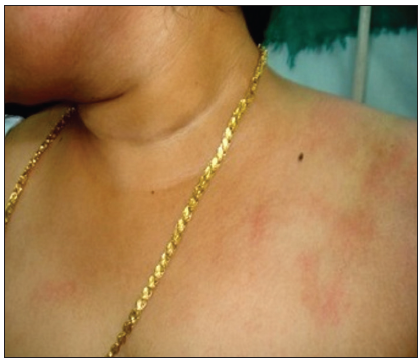
- Diffuse ill-defined erythematous rash involving the left side of the upper chest and lower half of face with few spillover lesions on the right side of the chest.
Her complete blood examination, urine analysis, peripheral smear, coagulation profile, and absolute eosinophil count were within normal limits. Serology for syphilis and human immunodeficiency virus infection was negative. A detailed virology workup on throat swab and serum was negative for infections due to Epstein– Barr, entero, corona, parvo B19, adeno, and human herpesviruses 6 and 7. Histopathological examination of the rash revealed mild acanthosis and spongiosis and sparse perivascular lymphocytic infiltrate in the dermis.
A final diagnosis of APE/unilateral laterothoracic syndrome was made.
We reassured the patient and treated her with cetirizine 10 mg daily and emollients for symptomatic relief. Eruption started fading in the 2nd week with scaling and completely subsided without any sequelae in 4 weeks.
In 1962, Brunner et al. described a new childhood exanthema that had a unilateral periflexural onset followed by a bilateral spread.[5] In 1993, Taieb et al. suggested the acronym APE of childhood.[6] The etiology of the rash remains unknown to this date. A viral etiology was proposed by many on the basis of the seasonal variations in occurrence (most cases appear during February–September) and the presence of non-specific prodrome including fever, upper respiratory tract (as observed in our patient), and digestive tract symptoms. However, on most occasions, confirmation was lacking as in our patient. This along with the absence of similar illness in family members and close contacts made many to suggest an inoculation disease hypothesis.[1,4]
In 50% of cases, rash will be associated with pruritus. Lymphadenopathy, when present, will be limited to the areas of initial eruption. Most published reports are in caucasians that too in the paediatric population. A female preponderance was described by many, but no sex predilection was noted by others.[1,4]
One interesting feature of the rash of our patient was the sparing of pressure points. A possible explanation could be the occlusion of capillaries, thus preventing the viral antigens from reaching the capillary loops and inciting inflammation.
APE is mostly a clinical diagnosis and laboratory investigations are generally not required. The characteristic histopathology of “perisudoral infiltration of lymphocytes” described in APE was missing in our patient.[1] Zawar has reported another case of APE in an adult which also lacked this specific histology.[4]
The common differential diagnoses include contact dermatitis, non-specific viral exanthems, drug-related eruptions, miliaria, superficial fungal infections, scabies, and atypical pityriasis rosea including giant and unilateral forms.[7,8]
A positive history of prodromal illness and a negative one of drug intake or contact with any chemicals or topical preparations before the onset of eruption, unilateral distribution, macular nature, sparse inflammatory cells on histology, and gradual resolution over 4 weeks were more suggestive of APE than an allergic contact dermatitis in our patient.
The disease is usually self-limiting in 4–6 weeks. Recurrences are reported rarely.[1]
This condition is often overlooked in adults due to its rarity and very few published Indian reports. We report this case to highlight its benign and self-limiting course so that unnecessary investigations and medications could be avoided.
Acknowledgment
We express our sincere gratitude to Dr. G Arun Kumar, Professor and Head, Manipal Centre for Virus Research for carrying out the virology workup.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent forms. In the form the patient(s) has/have given his/her/their consent for his/her/their images and other clinical information to be reported in the journal. The patients understand that their names and initials will not be published and due efforts will be made to conceal their identity, but anonymity cannot be guaranteed.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Asymmetric periflexural exanthem of childhood. Arch Dermatol. 1999;135:799-803.
- [CrossRef] [PubMed] [Google Scholar]
- Asymmetric periflexural exanthem in an adult. Clin Exp Dermatol. 2004;29:320-1.
- [CrossRef] [PubMed] [Google Scholar]
- Asymmetric periflexural exanthem in an adult. Acta Dermatol Venereol. 1997;77:79-80.
- [Google Scholar]
- Asymmetric periflexural exanthema: A report in an adult patient. Indian J Dermatol Venereol Leprol. 2003;69:401-4.
- [Google Scholar]
- A new papular erythema of childhood. Arch Dermatol. 1962;85:539-40.
- [CrossRef] [PubMed] [Google Scholar]
- Asymmetric periflexural exanthem of childhood. J Am Acad Dermatol. 1993;29:391-3.
- [CrossRef] [Google Scholar]





