Translate this page into:
Cultural dermatoses: A review
-
Received: ,
Accepted: ,
How to cite this article: Kannan RK. Cultural dermatoses: A review. J Skin Sex Transm Dis 2022;4:33-9.
Abstract
The impact of globalization and migration is reflected in cultural dermatoses which in earlier times were localized to specific regions. Therapeutic, cosmetic, and religious practices can lead to dermatoses. Therapeutic practices such as cupping, coining, acupuncture, and moxibustion may cause purpura and ecchymoses which are sometimes mistaken for child abuse. Cultural perception of beauty is often the motivation behind practices such as threading, use of bleaching agents, henna, bindi, and hair oils, which, in turn, can cause irritant and allergic contact dermatitis as well as a host of other dermatoses. Prayer nodules and turban dermatoses may manifest as outcomes of culture specific religious practices. A knowledge of these conditions can help the dermatologist to offer a correct diagnosis and treatment.
Keywords
Therapeutic
Cultural
Cupping
Coining
Henna
INTRODUCTION
Cultural influences play a significant role in medical disease and the skin is no exception. The current era of globalization has resulted in cultural exchanges cutting across geographical boundaries. Easy access to travel and intermingling of cultures have resulted in an interesting array of presentations to the physician. Dermatoses that arise out of cultural influences pose a significant challenge to dermatologists all over the world. The dermatologist must be aware of the host of morphologic presentations seen on the skin that may relate either to cosmetic or therapeutic purposes. This review attempts to elucidate a few of the common cultural dermatoses as the topic is fairly exhaustive.
DEFINITION
No formal definition has been noted in current literature. Cultural dermatology could be defined as the range of cutaneous manifestations that arise from treatments (done for therapy or for cosmetic appeal) that were influenced by the locally prevalent cultural practices.
DERMATOSES CAUSED BY THERAPEUTIC CULTURAL PRACTICES
Cupping
Cupping (Hijama in Arabic) is practiced in many countries in Asia, Latin America, and Eastern Europe and in Mexico as a therapy for a variety of diseases ranging from headache, indigestion, and acne to pneumonia.[1-3] The technique involves using a cotton ball soaked in alcohol and burning it inside a glass cup. The cotton ball is removed immediately before transferring the cup in an inverted position onto the body; the most common sites selected for this treatment are back, chest, abdomen, and buttocks. The lack of oxygen inside the cup creates a suction effect which damages the blood vessels in the papillary dermis.[4] This results in a circular erythema which later becomes edematous and then ecchymotic.[5] The proponents of this practice suggest that cupping exerts benefit by transferring the pathology from one area to another or by elimination of toxins by increasing the circulation.[3] Different variations of cupping practiced include using lubricants to move the cup (which may produce linear streaks of purpura), wet cupping that involves abrading the skin before cupping and modern cupping that uses suction devices to create negative pressure.[5] The lesions produced by cupping may sometimes be mistaken for child abuse.[6] Complications of cupping are panniculitis, burns, ulcer formation, koebnerization, hyperpigmentation, erythema ab igne, and suction blisters [Figure 1].[7]
- Multiple suction blisters on the right scapular area of a young girl after undergoing “cupping” treatment (Image courtesy - Dr. Karalikkattil T Ashique, DDVL; PGDHS; FRCP (London), Senior Consutlant Dermatologist, Amanza Skin Clinic, Perinthalmanna).
Acupuncture
Acupuncture is a form of traditional therapy popular in China and Japan. It involves the insertion of disposable sterile needles onto the acupoints over the skin and their stimulation by needle, heat, or pressure. The philosophy employed is to alter the vital energy (Qi) between the different organs. It is employed as a treatment for a variety of disorders including dermatological disorders such as acne, atopic dermatitis, psoriasis, chronic urticaria, varicella infection, and herpes zoster.[3,5] The adverse events are bleeding, purpura, ecchymoses, hematoma, localized argyria, and silica granulomas; very rarely serious events such as pneumothorax and anaphylaxis may occur.[3,8,9]
Moxibustion
Moxibustion or therapeutic burns is an unusual form of traditional therapy used in various Asian cultures.[2] The moxa herb (Mugwort, Artemisia vulgaris) is rolled into a cone and burned on the skin in direct moxibustion.[3,5] In indirect moxibustion, the moxa stick is lit near the skin or is burned over acupuncture needles.[5] Moxibustion is used to treat a variety of conditions ranging from fever, abdominal pain and verrucae to breech presentation, stroke rehabilitation and cancers. The most common complications are burns and the rare adverse events include blistering, pruritus, keloids, cellulitis, and abscess. The discrete circular or target-like burns resemble cigarette burns and hence may be misdiagnosed as signs of child abuse.[3]
Coining
Coining (Cao gio meaning scratch out the wind in Vietnamese) and spooning (Gua sha meaning scraping sand in Chinese) are practiced in various Asian cultures as a remedy for fever, headache, and chills.[10] The edge of a coin or spoon is vigorously rubbed on the oiled skin, until petechiae, purpura, or ecchymoses occur. Most often these appear in a pine tree pattern.[3] This practice is believed to get rid of all bad winds causing illness and the lesions can be mistaken for child abuse.[2]
Ayurvedic medicine
In India, Ayurveda is a way of life and Ayurvedic medicines, both topical and systemic are universally perceived to be without any side effects. Some Ayurvedic preparations contain toxic levels of lead, cadmium, and mercury and their ingestion may result in heavy metal toxicity.[3] Furthermore, arsenic can cause palmoplantar keratoderma, leukomelanoderma, arsenical keratosis, Bowen’s disease, and squamous cell carcinoma (SCC).[11] Mercury can cause gingivitis, stomatitis, and acrodynia.[12] Steroids in topical and systemic preparations alter the dermatological picture and can lead to weight gain, hypertrichosis, and depigmentation.[13] Topical preparations like “thailams” (Ayurvedic oils) have led to allergic contact dermatitis including exfoliative dermatitis and irritant contact dermatitis.[11,14,15] As part of aromatherapy, mustard, coconut, linseed, and gingelly oils are used, which may cause photosensitive reactions and perioral and intraoral dermatitis.[16] Oil of bergamot, popularly used in aromatherapy contains furocoumarins, mainly bergapten (5-methoxypsoralen), which can cause photo-toxicity.[17]
DERMATOSES CAUSED BY CULTURAL AND SOCIO-ECONOMIC PRACTICES
An understanding of the cultural and socio-economic practices of various cultures is an essential knowledge for the practicing dermatologist. The multitude of sociocultural and religious practices in a country of wide diversity, like India, can give rise to numerous dermatoses. Since this is an exhaustive topic only a few dermatosis relevant to the Indian scenario and that which may pose diagnostic dilemmas will be mentioned here.
Henna
Henna is commonly used to dye hair, nail, and skin (Mehndi). The active ingredient is Lawsone (2-Hydroxy-1,4-naphthoquinone). Henna is derived from the leaves and flowers of the plant Lawsonia inermis of the family Lythraceae. Henna is a popular agent used for tattooing (pseudo-tattooing) since it does not require skin piercing.[16] Henna is also used to dye leather and fur.[5] Pure henna (red henna) causes allergic reactions very rarely, but the adulterants in black henna (diaminotoluenes and diaminobenzenes like para-phenylenediamine [PPD]) are known to cause a variety of allergic reactions.[18] These are added for a deeper color and a quicker drying. Some of the allergic reactions to henna are listed in Table 1.[16,19-26]
| Eczematous contact dermatitis |
| Pustular contact dermatitis |
| Vesiculobullous lesions |
| Immediate hypersensitivity reactions with rhinitis, |
| conjunctivitis, urticaria |
| Angioedema |
| Pigmentary alterations (hypopigmentation, hyperpigmentation, and depigmentation) |
| Lichenoid reactions |
| Localized hypertrichosis |
| Scarring, keloids |
| Acute renal failure with renal tubular necrosis |
In glucose-6-phosphate dehydrogenase deficient individuals, especially individuals sensitized to PPD through exposure to hair or textile dyes, use of henna may result in oxidative hemolysis and hemolytic crisis. People allergic to henna should avoid henna products and PPD or its cross reactors such as latex rubber, azo dyes, sulfonamides, thiazide diuretics, and local anesthetics.[27]
Bindi
“Bindi” means dot or point in Sanskrit and denotes the decorative accessory worn by Indian women for socio-religious purposes. It has become more of a fashion accessory now.[5] Usually, vermilion (sindoor or kumkum) is used to put “Bindi.” Red colored sindoor contains red sulfide or mercury sulfide whereas the black paste contains lead sulfide.[28] Kumkum is made by adding slaked lime to turmeric.[29] Nowadays, artificial “stick-on” bindis are in vogue. These are made of polyvinyl chloride with an adhesive (usually para-tertiary-butyl-phenol [PTBP]).[30] Bindi dermatoses present as allergic contact dermatitis, pigmented contact dermatitis, leukoderma, foreign body granuloma, and lichen planus pigmentosus.[5,29,31] The contact dermatitis is commonly due to the nickel dyes such as Brilliant Lake Red R, Disperse blue 106, and Disperse blue 124, and chemical additives such as thimerosal and gallate mix.[6] PTBP is the culprit causing depigmentation in most of the cases.[30]
“Holi” dermatoses
“Holi,” the festival of colors is celebrated in India by splashing or spraying colors on people. The natural colors used in earlier times have been substituted by inexpensive, industrial dyes, nowadays. Some of the colors used and their ingredients are listed in Table 2.[32]
| Color | Chemical |
|---|---|
| Black | Lead oxide |
| Green | Copper sulfate, malachite green |
| Silver | Aluminum bromide |
| Blue | Prussian blue |
| Red | Mercury sulfate |
Mica dust is added to the powders to add sparkle and this often causes micro trauma.[32] Eczematous lesions are the most common among “Holi dermatoses.” Other manifestations of “Holi dermatoses” include erosions, xerosis, scaling, erythema, urticaria, nail fold inflammation, and secondary pyoderma. Ocular complications vary from the mild symptoms of redness, watering and grittiness to more serious conjunctivitis, corneal abrasions, and periorbital necrotizing fasciitis. Vigorous scrubbing to remove the colors can lead to abrasions, especially on the face. Pre-existing dermatoses such as acne vulgaris, eczema, and paronychia may sometimes flare-up. Strict regulations of the quality control of the powders used to play “Holi” are the call of the hour.[33]
Mudichood
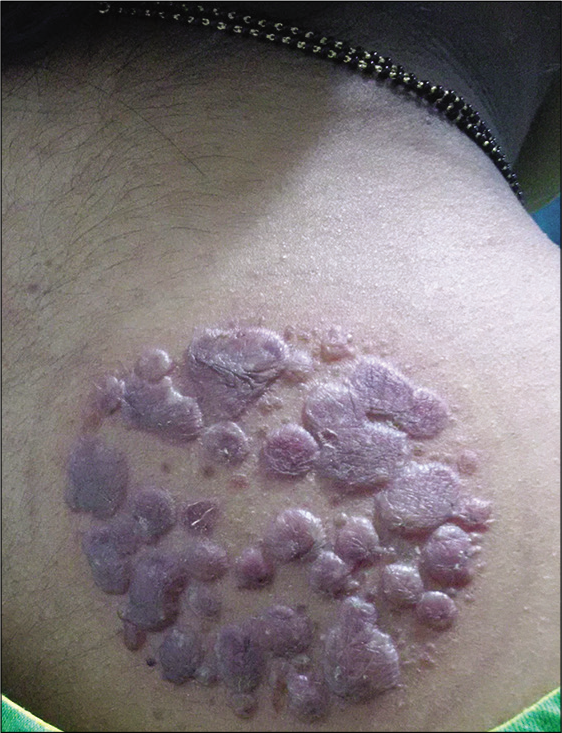
“Mudichood,” a condition first described from Kerala means heat of the hair in Malayalam. The sites commonly affected are the posterior neck and upper back. Lesions characteristically present as slightly hyper-pigmented, well defined, coin shaped, flat topped, and mildly pruritic follicular papules. These papules have a thin keratinous rim with a slightly depressed center. Removing the adherent scales leaves a hyper-pigmented base similar to lichen planus. Occasionally Koebner phenomenon is seen. Most often seen in young girls, mudichood is attributed to the customs of oiling the hair with plain or medicated coconut or sesame oil and leaving the hair untied after a bath. Mudichood is believed to be the response to heat, humidity and friction and subsides with topical 3–5% salicylic acid ointment. Mudichood can be prevented by avoiding excess oiling of hair and by frequent shampooing of hair [Figure 2].[34]

- Hyper-pigmented, flat topped, follicular papules of mudichood (Image courtesy - Dr Abhay Mani Martin. MD DVD, DNB Senior Consutlant Dermatologist, Baby Memorial Hospital, Kozhikode).
Drawstring dermatitis
Sari and Salwar are popular dresses in India and both require tying up at the waist, sometimes very tightly. This can lead to the formation of an artificial groove at the waist, more prominent in obese women, which is subjected to friction and pressure. Acute friction leads to the formation of blisters whereas chronic friction may result in a lichenified, hyperkeratotic, and hyperpigmented band. The trauma by rubbing results in the release of pro-inflammatory cytokines, growth factors, and adhesion molecules which cause post-inflammatory hyperpigmentation. This can also cause post traumatic depigmentation and koebnerization of preexisting vitiligo and lichen planus lesions. The occlusion by clothing, humid environment, sweating, and trauma by friction predispose to candidal, dermatophytic, and bacterial infections.[35] A case of Marjolin ulcer later becoming SCC termed “sari cancer” has also been reported.[27]
Hair oils
Hair oils commonly used in India are mustard oil, almond oil, amla oil, and coconut oil. Saturated and unsaturated fatty acids in these oils inhibit the growth of dermatophytes. Amla oil has maximum toxicity against Microsporum canis,Microsporum gypseum, and Trichophyton rubrum whereas coconut oil has maximum toxicity against Trichophyton mentagrophytes. The low incidence of tinea capitis in India is attributed to the widespread use of hair oils.[16] Hair oils can cause allergic contact dermatitis (pityriasis rosea – like eruptions), irritant dermatitis, and contact urticaria. Hair oils with a high oleic acid content such as coconut oil and olive oil may exacerbate seborrheic dermatitis as several species of Malassezia have high lipase activity and utilize the oils for their growth.[27]
Herbal oils
There are reports of chemical leukoderma following application of herbal oils including a case of leukoderma of breast after application of oil for breast massage.[36]
Hair restructuring and styling techniques
Heat, chemicals, and physical modalities are very much in vogue now as part of hairstyling procedures. Heating uses a metal comb heated to very high temperatures (150–500°F) and running it through the hair. Hair relaxers are chemicals containing sodium hydroxide, calcium hydroxide, guanine hydroxide, and formaldehyde derivatives. Both the heat and chemicals act by disrupting the disulfide bonds in keratin. Hair relaxers can cause chemical burns, contact dermatitis, hair shaft fragility and breakage, seborrheic dermatitis, hypo and hyperpigmentation of hair, scarring alopecia, and rarely Stevens-Johnson syndrome.[27] Pomade acne associated with the use of pomades on hair may manifest as perifollicular papules, pustules or closed comedones on the face.[6] Thermal straightening can produce moderate to severe burns and hair shaft damage.[27] Acquired trichorrhexis nodosa is another adverse event of these hair structuring techniques. The proximal variant is common in African Americans and appears as one or more nodes seen as white specks on the hair shaft. The distal variant is common in Caucasians and Asians and is associated with longitudinal splitting or split ends.[6]
Threading
Threading is a temporary method of removal of unwanted facial hair using a cotton thread and swift twisting movements of the hand when the thread is held fast in the mouth. The complications are usually pain, erythema, pruritus, edema, folliculitis, irritant dermatitis, and secondary pigment changes.[27] Infectious dermatoses such as bullous impetigo, plane warts, and molluscum contagiosum can occur at the threading sites.[37] The dermo-epidermal barrier disruption can result in seeding of the human papilloma virus leading to verrucae formation.
Melanocyte stem cell reservoir damage can occur by threading which may result in depigmentation.[16]
Prayer nodules
Prayer nodules are believed to be “religious equivalents of occupational callus.” Muslims pray 5 times a day mostly in squatting position.[16] The repeated friction results in lichenified hyper-pigmented nodules on the forehead, knees, ankles, and dorsum of feet.[38]
Contact dermatitis to “Rudraksha”
There have been case reports of contact dermatitis from necklaces made from beads of the holy basil (Ocimum sanctum) plant and seeds of the evergreen tree (Elaeocarpus ganitrus), the latter commonly known as “Rudraksha” [Figure 3].[38]
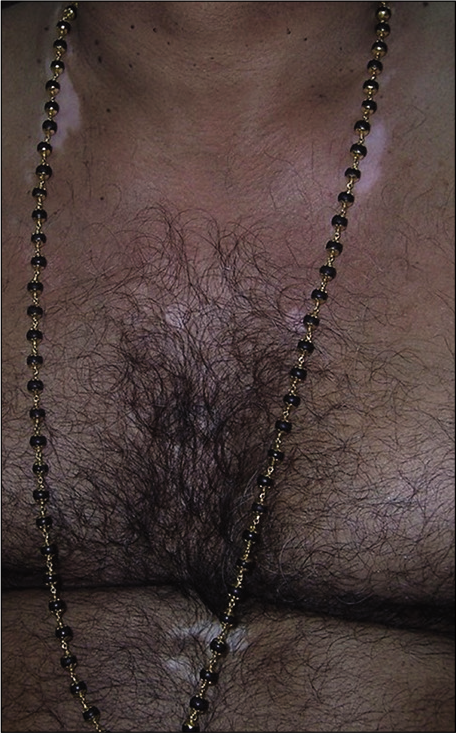
- Contact leukoderma to fake “Rudraksha” beads (Image courtesy - Dr Abhay Mani Martin. MD DVD, DNB, Senior Consutlant Dermatologist. Baby Memorial Hospital, Kozhikode).
Turban related dermatoses
Sikh men are prohibited from cutting their hair and so they tie it into a tight knot on the vertex over which a turban is worn. The beard hair is pulled into a tight knot under the chin. This persistent pull results in a sharply circumscribed band such as alopecia along the frontal hairline and sides of mandible.[16] It can also cause ridging and burrowing of the scalp resembling cutis verticis gyrata. Discoid lupus erythematosus-like lesions or painful chondrodermatitis of pinna due to pressure from wearing a starched turban is termed “turban ear.” Occasional cases may present with prominence of anti-helices of ear.[38]
Colored string
Colored strings are worn around the neck, arms, and waist in India, as part of cultural and religious practices. The friction and the chemicals in the string can cause linear leukoderma or allergic contact dermatitis.[36]
Toothpaste
Toothpaste can cause allergic contact dermatitis of the index finger as well as contact cheilitis. Contact dermatitis of the index finger is mostly seen in South East Asians who use the index finger to rub the toothpaste or tooth powder over the teeth.[36]
Bleaching agents
In India, the skin lightening cosmetic market constitutes 61% of the total dermatology market. The desire to acquire a fair color is universal and many youngsters fall prey to this. The three most common ingredients of bleaching agents are hydroquinone, mercury, and super potent topical steroids. Hydroquinone causes exogenous ochronosis, a paradoxical hyperpigmentation, as well as allergic and irritant contact dermatitis.[39] Corticosteroid abuse can result in various dermatoses such as perioral dermatitis, steroid acne, telangiectasia, atrophic striae, hyperpigmentation, rosacea, tinea incognito, and hirsutism. Furthermore, steroid addiction or “topical steroid dependent face” may appear on abrupt cessation of the topical steroid (mostly after prolonged use) and may present as rebound erythema, burning, and scaling of the face.[38] The mercury in bleaching agents may cause renal, neurological, and dermatological side effects that manifest as burning face, contact dermatitis, grey or blue-black facial discoloration, flushing, purpura, erythema, and gingivostomatitis.[40,41]
Decorative nose and ear piercing
Nose piercing has cultural significance in South East Asia. The common adverse effects are contact dermatitis, infections, keloid, and granuloma pyogenicum and severe reactions such as necrosis and collapse of nasal wall.[27,36] Ear piercing is a routine part of the cultural practices in India and may result in contact dermatitis, keloids, perichondritis, perichondrial abcess, and traumatic tears.[42]
Scarification and tattooing
Scarification and tattooing (popular in Africa) are done to indicate the rank in the society, the family, the clan or the tribe as well as for decorative purposes.[6] Gingival tattooing is commonly practiced by Ethiopian women whose gingiva are smeared with kohl powder and pierced with a needle. Complications include keloid, squamous cell carcinoma (SCC), and hepatitis B and C infections.[27]
Kangri cancer
Kangri cancer is a SCC that arises by keeping lighted coal in a kangri basket which is held close to the body, especially between the thighs or the lower abdomen, in winter, to keep the body warm. This is practiced mostly in remote hilly areas of Kashmir. The kangri basket contains lighted coal and dried chinar (Platanus orientalis) leaves. The cutaneous changes that begin as dyspigmentation, erythema ab igne, induration and thickening, later progress to exophytic growths, ulcers, and eventually carcinoma.[16]
CONCLUSION
Cultural and social beliefs and customs are part and parcel of every society. Migration and transportation have become so easy, nowadays, that no cultural practice may be thought of as strictly confined to any one region. Hence, a comprehensive knowledge of the various dermatoses related to the therapeutic and cultural practices go a long way in formulating a correct diagnosis and treatment.
Declaration of patient consent
Not required as patients identity is not disclosed or compromised.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- History of cupping (Hijama): A narrative review of literature. J Integr Med. 2017;15:172-81.
- [CrossRef] [Google Scholar]
- Conditions mistaken for child abuse: Part II. Pediatr Emerg Care. 1996;12:217-21.
- [CrossRef] [PubMed] [Google Scholar]
- Dermatoses caused by cultural practices: Therapeutic cultural practices. J Am Acad Dermatol. 2018;79:1-16.
- [CrossRef] [Google Scholar]
- Dermatoses secondary to Asian cultural practices. Int J Dermatol. 2012;51:372-9.
- [CrossRef] [PubMed] [Google Scholar]
- Suction bullae as a complication of prolonged cupping. Clin Exp Dermatol. 2006;31:300-1.
- [CrossRef] [PubMed] [Google Scholar]
- Adverse events in acupuncture and moxibustion treatment: A six-year survey at a national clinic in Japan. J Altern Complement Med. 1999;5:229-36.
- [CrossRef] [PubMed] [Google Scholar]
- Prospective studies of the safety of acupuncture: A systematic review. Am J Med. 2001;110:481-5.
- [CrossRef] [Google Scholar]
- New onset of linear purpura on the back: Coining therapy-associated ecchymoses. Cureus. 2020;12:e8833.
- [CrossRef] [Google Scholar]
- Arsenic and mercury intoxication due to Indian ethnic remedies. BMJ. 1993;306:506-7.
- [CrossRef] [PubMed] [Google Scholar]
- Chronic arsenic toxicity from Ayurvedic medicines. Int J Dermatol. 2008;47:618-21.
- [CrossRef] [PubMed] [Google Scholar]
- Effect of alternative medicinal systems and general practice. Int J Dermatol. 2007;46:46-50.
- [CrossRef] [PubMed] [Google Scholar]
- Allergic contact dermatitis following aromatherapy with valiya narayana thailam--an Ayurvedic oil presenting as exfoliative dermatitis. Contact Dermatitis. 2009;61:297-8.
- [CrossRef] [PubMed] [Google Scholar]
- Dermatoses due to quackery: A case snippet and concise review of literature. Indian J Dermatol. 2016;61:75-7.
- [CrossRef] [PubMed] [Google Scholar]
- Dermatoses due to Indian cultural practices. Indian J Dermatol. 2015;60:3-12.
- [CrossRef] [PubMed] [Google Scholar]
- Accidental bullous phototoxic reactions to bergamot aromatherapy oil. J Am Acad Dermatol. 2001;45:458-61.
- [CrossRef] [PubMed] [Google Scholar]
- Vesicular erythema multiforme-like reaction to para-phenylenediamine in a henna tattoo. Pediatr Dermato. 2008;25:201-4.
- [CrossRef] [PubMed] [Google Scholar]
- For the love of color: Plant colors and the dermatologist. Indian J Dermatol Venereol Leprol. 2020;86:622-9.
- [CrossRef] [PubMed] [Google Scholar]
- Contact dermatitis with severe scalp swelling and upper airway compromise due to black henna hair dye. Pediatr Emerg Care. 2011;27:745-6.
- [CrossRef] [PubMed] [Google Scholar]
- The extent of black henna tattoo's complications are not restricted to PPD-sensitization. Contact Dermatitis. 2006;55:57.
- [CrossRef] [PubMed] [Google Scholar]
- Persistent leukoderma after henna tattoo. Contact Dermatitis. 2007;56:108-9.
- [CrossRef] [PubMed] [Google Scholar]
- Lichenoid reaction to temporary tattoo. Contact Dermatitis. 2000;42:117-8.
- [CrossRef] [Google Scholar]
- Severe inflammatory and keloidal, allergic reaction due to para-phenylenediamine in temporary tattoos. Indian J Dermatol Venereol Leprol. 2010;76:165-7.
- [CrossRef] [PubMed] [Google Scholar]
- Allergic contact dermatitis from henna. Contact Dermatitis. 1988;18:55-6.
- [CrossRef] [PubMed] [Google Scholar]
- Dermatoses caused by cultural practices: Cosmetic cultural practices. J Am Acad Dermatol. 2018;79:19-30.
- [CrossRef] [PubMed] [Google Scholar]
- Cultural dermatoses: Turmeric allergy (mangalsutra dermatitis and kumkum dermatitis) a case report. J Skin Sex Transm Dis. 2020;2:49-51.
- [CrossRef] [Google Scholar]
- Contact depigmentation by adhesive material of bindi. Contact Dermatitis. 1991;24:310-1.
- [CrossRef] [PubMed] [Google Scholar]
- Importance of cultural dermatology in India. Int J Dermatol. 2015;54:237-9.
- [CrossRef] [PubMed] [Google Scholar]
- The “Holi” dermatoses: Annual spate of skin diseases following the spring festival in India. Indian J Dermatol. 2009;54:240-2.
- [CrossRef] [PubMed] [Google Scholar]
- Cultural practice and dermatology: The “Holi” dermatoses. Int J Dermatol. 2012;51:1385-7.
- [CrossRef] [PubMed] [Google Scholar]
- Dermatological signs in South Asian women induced by sari and petticoat drawstrings. Clin Exp Dermatol. 2010;35:459-61.
- [CrossRef] [PubMed] [Google Scholar]
- Dermatoses secondary to Indian cultural practices. Int J Dermatol. 2014;53:e288-9.
- [CrossRef] [PubMed] [Google Scholar]
- Dermatoses due to Arabic cultural and traditional practices. Indian J Dermatol Venereol Leprol. 2019;85:448-54.
- [CrossRef] [PubMed] [Google Scholar]
- A 15-year-old girl with painful, peeling skin. Pediatr Ann. 2015;44:195-7.
- [CrossRef] [PubMed] [Google Scholar]
- Topical corticosteroid abuse on the face: A prospective, multicenter study of dermatology outpatients. Indian J Dermatol Venereol Leprol. 2011;77:160-6.
- [CrossRef] [PubMed] [Google Scholar]
- Mercury “bleaching” creams. J Am Acad Dermatol. 2005;52:1113-4.
- [CrossRef] [PubMed] [Google Scholar]






