Translate this page into:
Psychiatric comorbidities in patients with prurigo nodularis – A cross-sectional study from a tertiary care center in South India
*Corresponding author: Ettappurath N. Abdul Latheef, Department of Dermatology and Venereology, Government Medical College, Kozhikode -673008, Kerala, India. drlatheef90@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Krishnan LT, Latheef EN, Tharayil HM. Psychiatric comorbidities in patients with prurigo nodularis – A cross-sectional study from a tertiary care center in South India. J Skin Sex Transm Dis 2022;4:79-82.
Dear Editor,
The association between skin and the nervous system is related to their common embryonic origin, the ectoderm of fetus. They remain closely interconnected and interactive throughout the life.[1] The neural receptors in the skin are the largest sense organ of the body and are key to skin protection and health.[2] Pruritus or itch is one of the most common symptoms of dermatological disorders. Mind and pruritus are intertwined in a complex manner.[3]
Depression is a chronic or recurrent affective disorder usually associated with a physical morbidity. Depressive disorders are present in almost 30%–50% of dermatological patients.[4,5] Major depressive disorder (MDD) is characterized by one or more major depressive episodes lasting at least 2 weeks characterized by depressive mood (almost whole day or nearly every day) and markedly decreased pleasure, or interest in all or almost all activities.[6] Depending on the severity and number of symptoms, depression can be divided into mild, moderate, and severe.[7]
According to American psychological association “Anxiety is an emotion characterized by feelings of tension, worried thoughts and physical changes like increased blood pressure.” People with anxiety usually avoid certain situations that cause worry to them. They have recurrent intrusive thoughts or concerns and they experience physical symptoms such as sweating, trembling, dizziness, or palpitation.[8] Occasional anxiety is an unavoidable part of life, but anxiety disorders include more a than transient worry or fear. The symptoms interfere with daily activities of life such as school, work, and relationships. There are different types of anxiety disorders including generalized anxiety disorder, panic disorder, and various phobias.[8]
Dissociative disorders are characterized by lack of normal integration of thoughts, feelings, and experiences into the stream of consciousness and memory. It occurs on a continuum ranging from minor normative dissociations to psychiatric conditions.[9] These symptoms increase with severity of dissociation.[8] Itching is an important cutaneous symptom in dissociation.[9,10]
Prurigo nodularis (PN) and lichen simplex chronicus (LSC) are chronic psychogenic pruritic disorders characterized by intense pruritus, which may be intensified or perpetuated by emotional factors and are associated with intrinsic factors, such as local cytokine releases, neuropeptide changes, and inflammatory cell infiltrates.[11] Patients with PN and LSC have a high frequency of psychiatric morbidity, deranged sleep patterns, mood disturbances, anxiety, and depression which, in turn, exacerbate the itching.[12-14] Pruritus itself can significantly impair the quality of life and sleep.[15]
In this cross-sectional study, we assessed the psychiatric comorbidities of depression, anxiety, and dissociative experiences in patients with PN. The study was conducted in the outpatient dermatology department of a tertiary referral center after getting ethics committee approval. 60 consecutive patients with a clinical diagnosis of PN diagnosed (by a qualified dermatologist) and were of the age group between 13 and 70 years were included in the study. Patients with other medical illnesses, mental retardation, and other severe cognitive dysfunction interfering with the formal assessment were excluded from the study. Individual study participant gave written informed consent. Study period was 10 months, starting from May 2016 to February 2017. A pre-set questionnaire was used to collect socio-demographic parameters and dermatological features of the patients. Psychiatric morbidity was assessed by the following tools:
Mini international neuropsychiatric interview (MINI): It is a short, structured diagnostic interview developed in 1990 to explore the occurrence of major axis I psychiatric disorders and has high validity and reliability scores.[16]
The patient health questionnaire 9 (PHQ-9) is a nine-item depression module from the primary care evaluation of mental disorders corresponding to the diagnostic and statistical manual of mental disorder 4th edition major depressive criteria.[17]
The dissociative experiences scale (DES) is a tool used extensively to screen for dissociative symptoms.[18]
Vernacular (Malayalam) version of MINI, PHQ-9, and DES was administered in all patients and the scores were recorded. Illiterate patients who cannot read and respond by themselves, completed the proforma with the help of the investigator. The collected data were analyzed by frequency and percentage.
The results of 60 patients with PN were analyzed [Table 1, Figures 1 and 2]. The mean age was 37.9 years. 42 (70%) patients were females. Majority of the patients were married (36, 60%). 46 (76.7%) had secondary school education. Majority of the patients belonged to below poverty line.[19] 43 (71.7%) patients were from rural areas. 42 (70%) patients were from nuclear families. 26 (43.3%) were house wives and 17 (28.3%) were students. All patients had multiple lesions. Their size varied from few millimeters to many centimeters. Thirty (50%) patients had lesion of size 0.5–1 cm, 26 (43.3%) had lesions of size 1–1.5 cm, and 4 (6.7%) had lesions of size 1.5–2 cm. The most common affected area was lower limb followed by upper limb. 14 (23.3%) patients were on psychotropics for different psychiatric comorbidities. Out of these, 7 (11.6%) had lesions of size 1–1.5 cm. However, the rest had lesions of lesser size (0.5–1 cm). The mean duration of the illness was 6 months. No significant correlation was seen between the size of the lesion and the duration of the illness (correlation coefficient r = 0.213). Among the patients, 20 (33.3 %) were having some psychiatric comorbidity [Table 2]. Of this, 9 (9/60, 15%) had MDD, 6 (6/10, 10%) had history of MDD, 1 (1/60, 1.7%) had generalized anxiety disorder (GAD), and 1 (1/60, 1.7%) had social phobia. Three patients (3/60, 5%) had dysthymia. 40 (40/60, 66.7%) were without any psychiatric comorbidities. Mean PHQ-9 value was 2.75 and mean DES score was 1.09.
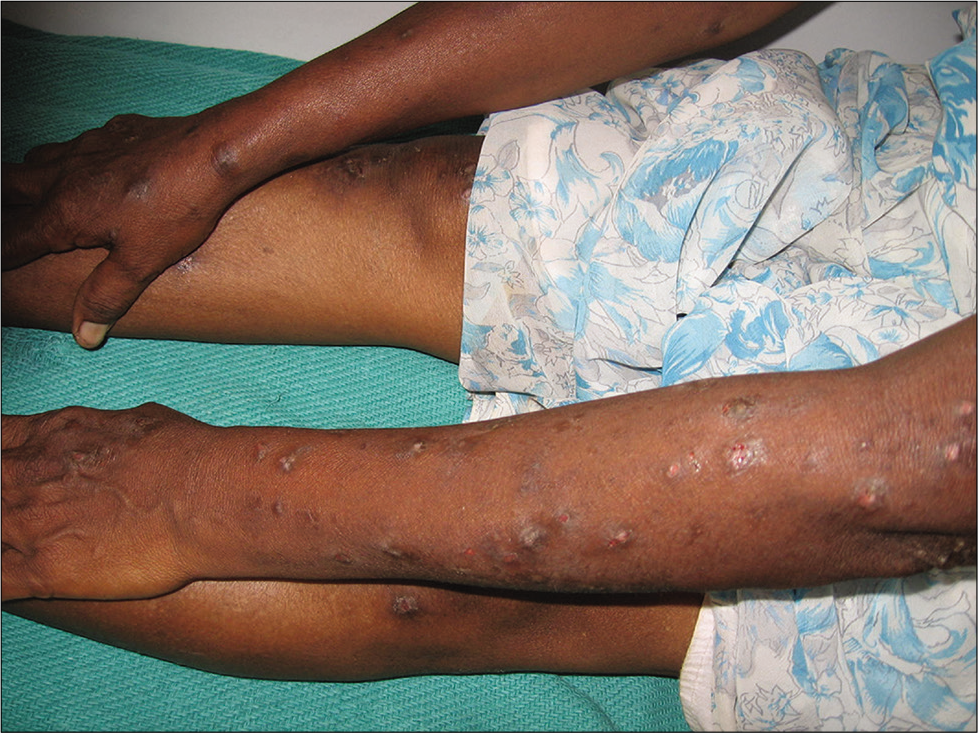
- Prurigo nodularis in an old lady.
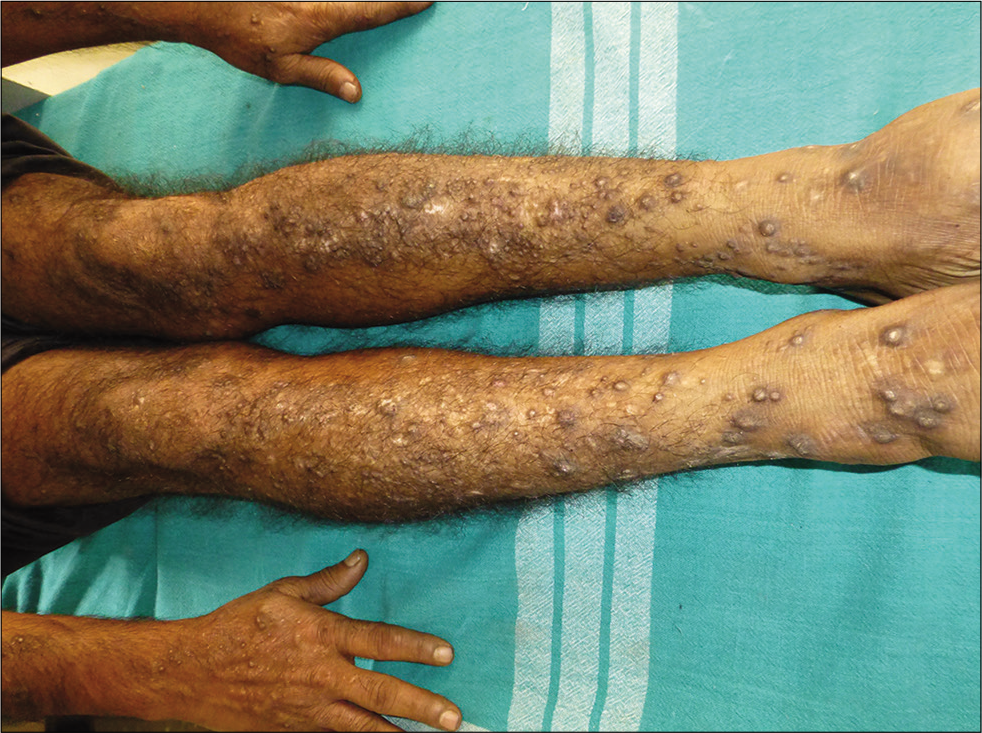
- Prurigo nodularis in a young man.
| S. No. | Socio-demographic details | Frequency(Percentage) |
|---|---|---|
| 1 | Sex | |
| Male | 18 (30) | |
| Female | 42 (70) | |
| 2 | Marital status | |
| Single | 19 (31.7) | |
| Married | 36 (60) | |
| Widow | 4 (6.7) | |
| Separated | 1 (1.7) | |
| Living together | 0 | |
| 3 | Education | |
| Not formally educated | 2 (3.3) | |
| Below 10thstandards | 46 (76.7) | |
| 11 and 12thstandards | 8 (13.3) | |
| Degree and higher | 4 (6.7) | |
| 4 | Occupation | |
| Unemployed | 8 (13.3) | |
| House wife | 26 (43.3) | |
| Unskilled | 3 (5) | |
| Semiskilled | 3 (5) | |
| Skilled | 3 (5) | |
| Student | 17 (28.3) | |
| 5 | Socioeconomic status | |
| Above poverty line | 17 (28.3) | |
| Below poverty line | 43 (71.7) | |
| 6 | Residence | |
| Rural | 40 (66.7) | |
| Urban | 20 (33.3) | |
| 7 | Type of family | |
| Nuclear | 42 (70) | |
| Joint | 9 (15) | |
| Extended | 9 (15) |
| Psychiatric comorbidity (MINI) | Frequency (%)n = 60 (100%) |
|---|---|
| Generalized anxiety disorder | 1 (1.7) |
| MDD | 9 (15) |
| Past history of MDD | 6 (10) |
| Social phobia | 1 (1.7) |
| *None | 40 (66.7) |
MINI: Mini international neuropsychiatric interview, MDD: Major depressive disorder. *Three patients had dysthymia that cannot be assessed by MINI.
In the present study, we observed that the mean age of the PN patients was 37.9 years. This finding was comparable to the previous studies.[20,21] The female preponderance noted by us was discordant to certain studies that reported an equal distribution in both sexes.[22] The most common affected area was lower and upper limbs. This was consistent with the observation of Rowland-Payne et al.[23] Our study could not find a significant relationship between the size of the lesion, extent of the lesion, and the duration of the illness. The lesions were more common in married females of poor socio-economic status, belonging to rural areas. Whether there is an actual relationship between the extent of PN and the socio-economic status or it is a reflection of the profile of the population seeking treatment in a government institution needs analysis in multicenter studies.
The psychiatric comorbidity noted in one-third of our study participants was higher than the same documented in the general population of the country (56/1000 population); but was comparable to the findings of the previous studies on PN.[13,24-28] Literature states depression as the most common psychiatric disorder associated with PN followed by anxiety disorder.[23] Our study also showed depression and anxiety as the common psychiatric comorbidities. Rowland-Payne et al. observed that 50% of patients had depression, anxiety, and other psychiatric disorders out of which 33% needed treatment.[23] Schneider et al. revealed a higher prevalence of alexithymia, somatization symptoms, hypochondriasis, anxiety, and depression.[21] Study by Konuk et al. observed higher frequency of psychiatric symptoms in LSC patients.[12] Contrary to the literature, none of our patients had dissociative experiences.[19] Dysthymia noted in three patients could not be assessed with MINI which was consistent with current knowledge.[29]
Single center study design and small sample size were the limitations.
Our findings suggest that one-third of the PN patients had some level of psychiatric comorbidity. MDD was the most common, followed by GAD and social phobia. This study could not find a relationship between dissociative experiences and PN. We suggest that a holistic approach may be required in the management of PN.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Psychodermatology has come out of its infancy. Dermatol Psychosom. 2004;5:3-4.
- [CrossRef] [Google Scholar]
- Personality differences between patients with lichen simplex chronicus and normal population: A study of pruritus. Eur J Dermatol. 2010;20:359-63.
- [CrossRef] [PubMed] [Google Scholar]
- Relaxation therapy in the management of psoriasis. Dermato Ther 2020:e14030.
- [CrossRef] [PubMed] [Google Scholar]
- Comorbidity of depressive and dermatologic disorders therapeutic aspects. Psychiatr Danub. 2009;21:401-10.
- [Google Scholar]
- Psychotherapy for major depressive disorder and generalized anxiety disorder: A health technology assessment. Health Technol Assess Ser. 2017;17:1-167.
- [Google Scholar]
- Use of mental health services for anxiety, mood, and substance disorders in 17 countries in the WHO world mental health surveys. Lancet. 2007;370:841-50.
- [CrossRef] [Google Scholar]
- Encyclopedia of Psychology Washington, DC, United States: American psychology Association; 2012. p. :3434-5.
- [Google Scholar]
- Somatisation in patients with dissociative disorders. Am J Psychiatry. 1994;151:1329-13.
- [CrossRef] [PubMed] [Google Scholar]
- Medically unexplained cutaneous sensory symptoms may represent somatoform dissociation: An empirical study. J Psychosom Res. 2006;60:131-6.
- [CrossRef] [PubMed] [Google Scholar]
- Lichen simplex chronicus, neurotic excoriation and nodular prurigo and their correlation with atopy: A case-control study. Iran J Dermatol. 2011;14:25-8.
- [Google Scholar]
- Psychopathology, depression and dissociative experiences in patients with lichen simplex chronicus. Gen Hosp Psychiatry. 2007;29:232-5.
- [CrossRef] [PubMed] [Google Scholar]
- psychological factors in prurigo nodularis in comparison with psoriasis vulgaris: Results of a case-control study. Br J Dermatol. 2006;154:61-6.
- [CrossRef] [PubMed] [Google Scholar]
- Association between frequency of pruritic symptoms and perceived psychological stress: A Japanese population based study. Arch Dermatol. 2009;145:1384-8.
- [CrossRef] [PubMed] [Google Scholar]
- The prevalence and clinical characteristics of pruritus among patient with extensive psoriasis. Br J Dermatol. 2000;143:969-73.
- [CrossRef] [PubMed] [Google Scholar]
- The mini-international neuropsychiatric interview (M.I.N.I.): THE development and validation of a structured diagnostic psychiatric interview for DSM-IV and ICD-10. J Clin Psychiatry. 1998;59(Suppl 20):22-33. quiz 34-57
- [Google Scholar]
- The PHQ-9: Validity of a brief depression severity measure. J Gen Intern Med. 2001;16:606-13.
- [CrossRef] [PubMed] [Google Scholar]
- Development, reliability and validity of a dissociation scale. J Nerv Ment Dis. 1986;174:727-35.
- [CrossRef] [PubMed] [Google Scholar]
- Poverty and food security in Gujarat, India. Eur J Dev Res. 2011;23:129-50.
- [CrossRef] [Google Scholar]
- Psychosomatic aspects and psychiatric conditions Pruritus. London: Springer-Verlag; 2010. p. :211-5.
- [CrossRef] [Google Scholar]
- Central activation by histamine-induced itch: Analogies to pain processing: A correlational analysis of O-15 H(2) Opositron emission to mography studies. Pain. 2001;92:295-305.
- [CrossRef] [Google Scholar]
- Nodular prurigoa clinico pathological study of 46 patients. Br J Dermatol. 1985;113:431-9.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence of mental disorders in India and other South Asian countries. Asian J Epidemiol. 2017;10:45-53.
- [CrossRef] [Google Scholar]
- Psychogenic excoriation. Clinical features proposed diagnostic criteria, epidemiology and approaches to treatment. CNS Drugs. 2001;15:351-9.
- [CrossRef] [PubMed] [Google Scholar]
- Obsessive compulsive disorder in patients with chronic pruritic conditions: Case studies and discussion. J Am Acad Dermatol. 1992;26:549-51.
- [CrossRef] [Google Scholar]
- Cognitive and emotional influences in anterior cingulate cortex. Trends Cogn Sci. 2000;4:215-22.
- [CrossRef] [Google Scholar]
- The mini international neuropsychiatric interview is useful and well accepted as part of the clinical assessment for depression and anxiety in primary care: A mixed methods study. BMC Fam Pract. 2018;19:19.
- [CrossRef] [PubMed] [Google Scholar]





