Translate this page into:
Atypical manifestations of atopic dermatitis
*Corresponding author: Ram Gulati, Department of Dermatology, SDM Hospital, Jaipur, Rajasthan, India. dr_ramgulati@yahoo.com
-
Received: ,
Accepted: ,
How to cite this article: Gulati R. Atypical manifestations of atopic dermatitis. J Skin Sex Transm Dis 2021;3:118-24.
Abstract
Atopic dermatitis or atopic eczema is a complex heterogeneous inflammatory skin condition, typified by classic distribution pattern in most cases. Typically, in infancy it involves the cheeks, and over time, as it settles over the cheek area, extensors tend to get involved, and by 2 years of age flexural distribution predominates. Acral pattern is largely seen in adult population but may unusually be seen in children. This review article focuses on the atypical manifestations of atopic dermatitis.
Keywords
Atopic dermatitis
Atopic eczema
Atypical manifestations
Acral dermatitis
Lichenoid atopic dermatitis
INTRODUCTION
Atopic dermatitis or atopic eczema is a complex, heterogeneous inflammatory skin condition, typified by classic distribution pattern in most cases. Typically, in infancy it involves the cheeks, and over time, as it settles over the cheek area, extensors tend to get involved, and by 2 years of age flexural distribution predominates. Acral pattern is largely seen in adult population but may unusually be seen in children. Lacking a reliable definitive biomarker, diagnosis of atopic dermatitis is largely based on clinical features. In 1980, Hanifin and Rajka enumerated diagnostic features of atopic dermatitis, whereby four basic and 23 minor criteria were proposed, and presence of at least three basic and three minor criteria was needed for a firm diagnosis.[1] As this was an exhaustive list, over time, various dermatology study groups came up with modifications either to simplify or standardize it further.[2] Hanifin and Rajka criteria, though found to have high sensitivity and utility in children, were found to be quite cumbersome to administer.[3,4] Simpler criteria like the UK Working Party Group criteria tend to focus on the typical signs and symptoms, making it easy for routine practical clinic usage, but miss out on the less common atypical manifestations of atopic dermatitis.[5] In fact, if we carefully dissect the Hanifin and Rajka criteria, many of the minor ones represent the findings of careful observation of a large cohort by the panelists who mulled over it when formulating the criteria, whereby it was intended to include even those cases which presented with less common manifestations. Over the next 40 years, other authors have corroborated these findings and have added other less common presentations too. This heterogeneity and diversity in presentation of atopic dermatitis are in fact, the prime reason for evolution of multiple diagnostic criteria over past so many decades, with hardly any one set covering the entire spectrum of the disease. Significant difference exists in clinical presentation between patients who are seen in hospital setting versus community setting with moderate-to-severe disease prevalent in the former and mild-to-moderate disease in the latter.[2,6,7]
Scanning the available literature provides us with the following list of atypical manifestations of atopic dermatitis:[8-10]
Lichenoid atopic dermatitis
Nummular-type atopic dermatitis
Psoriasiform atopic dermatitis
Follicular atopic dermatitis
Juvenile plantar dermatosis
Lip licker’s dermatitis
Nipple eczema
Atopic dermatitis of scalp
Alopecia of atopic dermatitis
Perianal and perineal atopic dermatitis
Eyelid eczema
Genital eczema
Retroauricular eczema
Rhagades of nasal orifices
Finger pad eczema
Atopic hands and feet
Eczema coxsackium.
Let us look at these less common or unusual manifestations in some detail:
LICHENOID ATOPIC DERMATITIS OR LICHEN PLANUS LIKE ATOPIC DERMATITIS
This variant presents as intensely pruritic, skin colored to erythematous flat-topped papules [Figure 1] in an extensor distribution on the limbs.[11] More common in children, this variant tends to decrease with age and is seen more commonly in summer.[10] Histopathology may be needed to differentiate it from lichen planus, as it shows spongiotic dermatitis rather than lichenoid infiltrate. If contact allergy is suspected, patch testing may help. Topical therapy may suffice but if extensive or not settling, phototherapy should be considered. Resistant lesions may respond to short course of wet wrapping.
- Lichenoid atopic dermatitis involving the elbow region.
NUMMULAR-TYPE ATOPIC DERMATITIS
On the background of atopic dermatitis, this presents with discoid eczematous plaques which may show oozing and lichenification [Figure 2].[8,10] The lesions usually affect the extensor extremities especially wrists and ankles, though other areas can be affected too.[12] It may develop subsequent to a reaction to a nidus like molluscum lesions.[13] Patch testing may help if clinically indicated, and some authors suggest patch testing all cases of chronic recalcitrant nummular dermatitis.[14,15] Lesions tend to be stubborn and may need proactive treatment with topical steroids or calcineurin inhibitors.
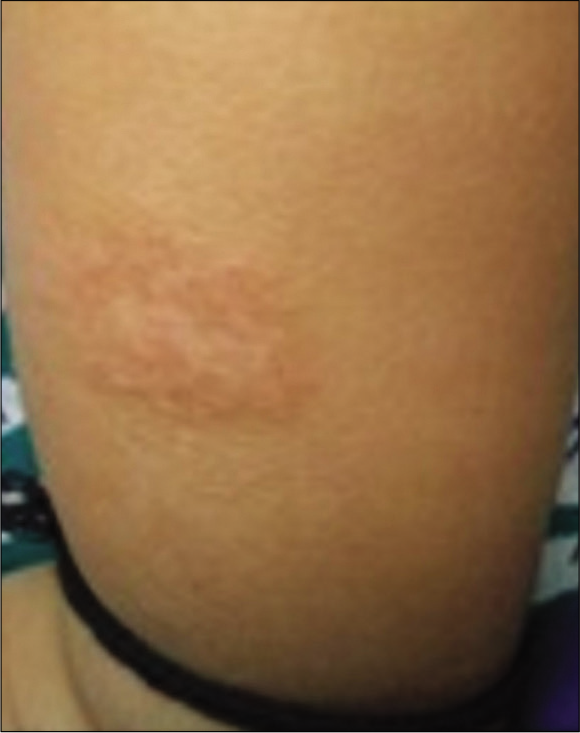
- Nummular type atopic eczema.
PSORIASIFORM ATOPIC DERMATITIS
Often presenting as treatment resistant plaques, this may represent an overlap with psoriasis or a psoriasiform contact reaction or a result of both Th17 and Th2 activation, which is more commonly seen in Asians.[16] It more commonly affects scalp and diaper area [Figure 3].[16] Psoriasiform dermatitis often needs phototherapy or systemic treatment. Considering the role of interleukin-23/Th17, ustekinumab is considered as a potential targeted therapy.

- Psoriasiform atopic dermatitis, perifollicular accentuation visible in surrounding skin.
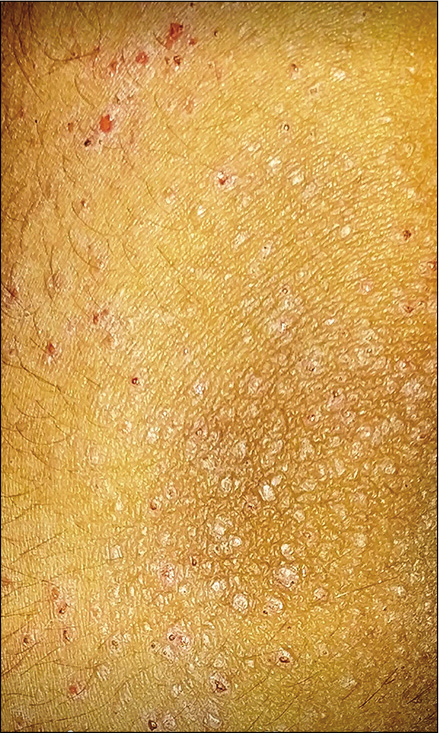
FOLLICULAR ATOPIC DERMATITIS
Follicular variant is more commonly seen in Asian ethnicity, though other ethnic groups are affected too.[17] Hanifin and Rajka mentioned perifollicular accentuation as one of the minor criteria.[1] Intense itching on what looks like normal skin to the family, is the usual presentation; however, careful examination shows follicular prominence mostly across the chest, abdomen, back, and proximal extremities. It tends to show seasonal variation with more prominence in winters.[10] Histopathology tends to show typical spongiotic dermatitis affecting follicular and perifollicular epithelium.[17] Prolonged course of moderate to potent topical steroids repeated as needed, or phototherapy is usually needed.
JUVENILE PLANTAR DERMATOSIS
Presenting usually in school going children, this manifests as pruritic erythematous glazed shiny, but scaly skin affecting the plantar areas, usually the forefoot [Figure 4] and sometimes only the great toe to start with.[18] Summer exacerbation is noted, and therefore, role of hyperhidrosis and occlusive footwear such as one made from plastic is emphasized.[19] Contact dermatitis to shoes should be ruled out, especially if there is temporal relationship to wearing of new footwear or if other areas of feet such as the dorsa or heel are affected.[20,21] Emollients stay as the mainstay of management though intermittent use of moderate to potent topical steroids may be needed. Topical calcineurin inhibitors can be used as steroid sparing agents.[22] Excessive sweating of feet should be addressed and occlusive footwear should be avoided. Condition mostly tends to resolve post puberty.
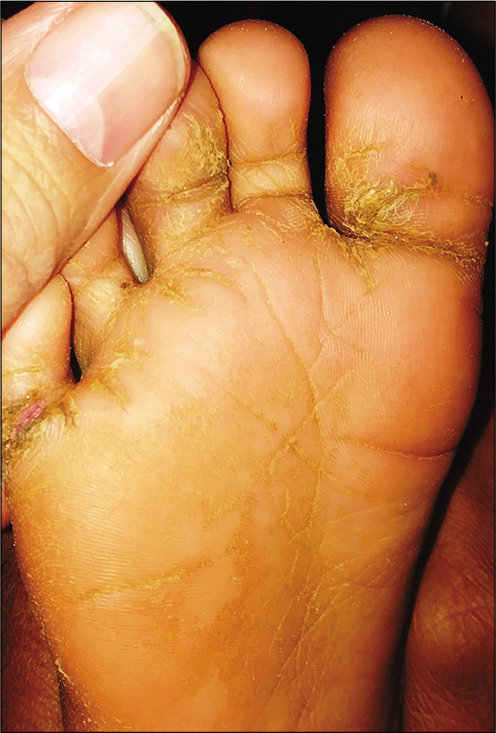
- Juvenile plantar dermatosis.
LIP LICKER’S DERMATITIS
Atopic dermatitis can present as inflammation affecting the lips and surrounding area. As these lesions feel dry, patients unwittingly start licking the lips to moisten them. However, this spirals into a vicious cycle with saliva eventually exacerbating the dryness and inflammation, referred to as lip licker’s dermatitis.[12,23] Clinically, it is seen as a well demarcated eczematous area affecting the lips and surrounding area [Figure 5]. If clinical history suggests or if persistent or recurrent, food allergy, and contact allergy should be ruled out.[24] Regular emollient with short course of topical mild-to-moderate potency corticosteroid is usually helpful.[12,23] If persistent, then proactive use of topical calcineurin inhibitor is safer. Post-inflammatory pigmentation may take a few weeks or longer to settle.
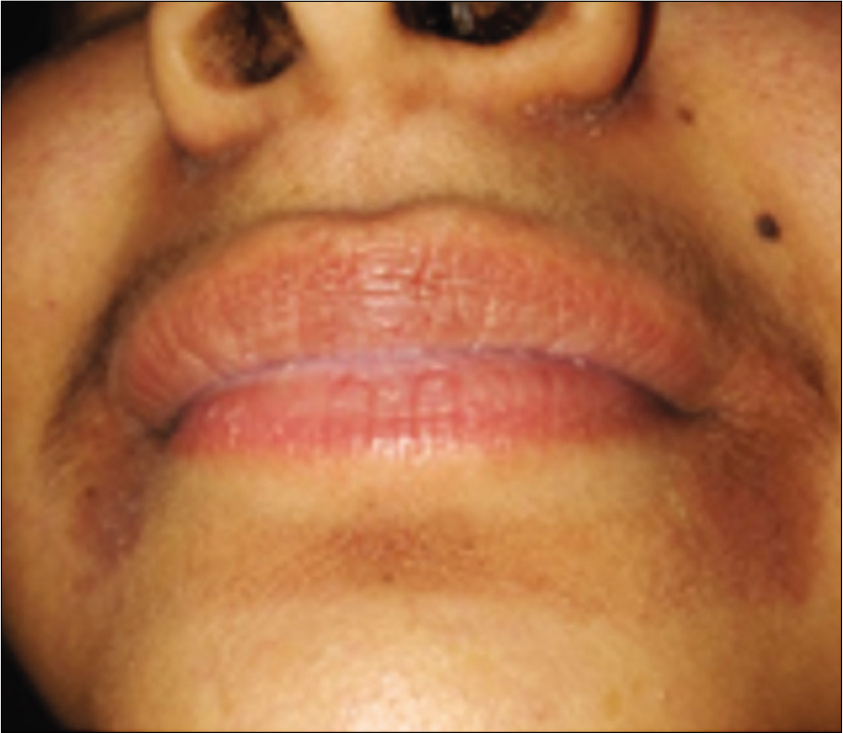
- Lip licker’s dermatitis.
NIPPLE ECZEMA
Part of minor criteria by Hanifin and Rajka, this localized variant has been considered to be an unusual presentation of atopic eczema.[1] A prospective study comprising of 195 patients showed nipple eczema to be statistically highly significantly associated with atopic eczema.[25] It usually presents in adolescence, affecting nipple and areolar area bilaterally, though unilateral cases have been described too [Figure 6].[26,27] If persistent and/or recurrent, and especially if affecting peri-areolar area, allergic contact dermatitis should be ruled out.[26]
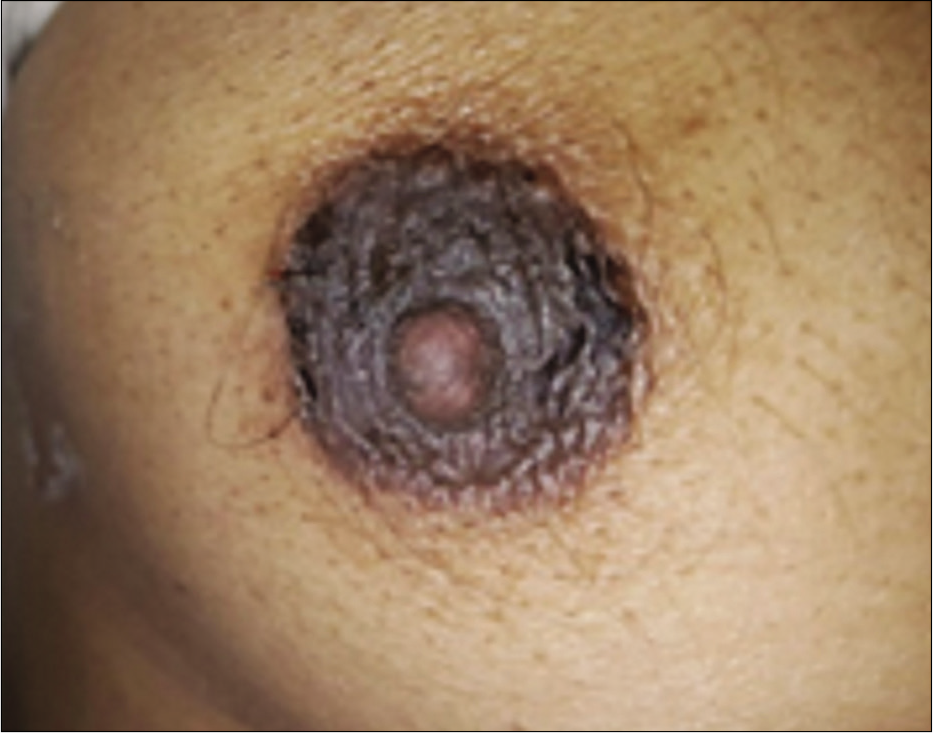
- Nipple eczema.
ATOPIC DERMATITIS OF SCALP[28]
Dermatitis of the scalp in atopic dermatitis can be a reaction to Pityrosporum; however, atopic dermatitis of the scalp has been described as a rare manifestation.[29] Seborrheic dermatitis of the scalp, which is more common, remains an important differential. The presence of scales on other seborrheic sites and greasy nature of scales do help in diagnosing the latter.
ALOPECIA OF ATOPIC DERMATITIS
An integral part of Netherton’s syndrome, alopecia has also been linked to atopic dermatitis by many authors.[30] This is usually seen on the margins of the scalp over excoriated eczematous areas and can be accompanied by xerosis of the hair shafts.[8] Persistent friction produced by rubbing of these areas leads to loss of hair. Bland vegetable oils can be used to moisturize the scalp. Foam based or aqueous based corticosteroid preparations should be used as alcohol based preparations can exacerbate dryness and cause irritation. Once eczema settles, alopecia tends to recover over time.
PERINEAL AND PERIANAL ATOPIC DERMATITIS
Dermatitis affecting perianal and perineal areas [Figure 7] has a wide differential including psoriasis, lichen sclerosus, infections, allergic contact dermatitis, and irritant contact dermatitis. The presence of friction, heat, and humidity in an occluded pelvic area changes the morphology making a correct diagnosis difficult.[31] Fecal contamination, repeated washing, rubbing or scratching can cause exacerbation of symptoms, while exposure to Staphylococci and Streptococci can lead to perianal bacterial dermatitis, especially in children.[32] Patch testing should be considered in patients with history suggestive of a contact reaction or in persistent cases.[33] Background history of atopy can help in pointing toward the possibility of atopic dermatitis. Although localized treatment with emollients, topical corticosteroids and calcineurin inhibitors are the usual modality, persistent lesions, especially if associated with unremitting pruritus may warrant the use of immunosuppressants.
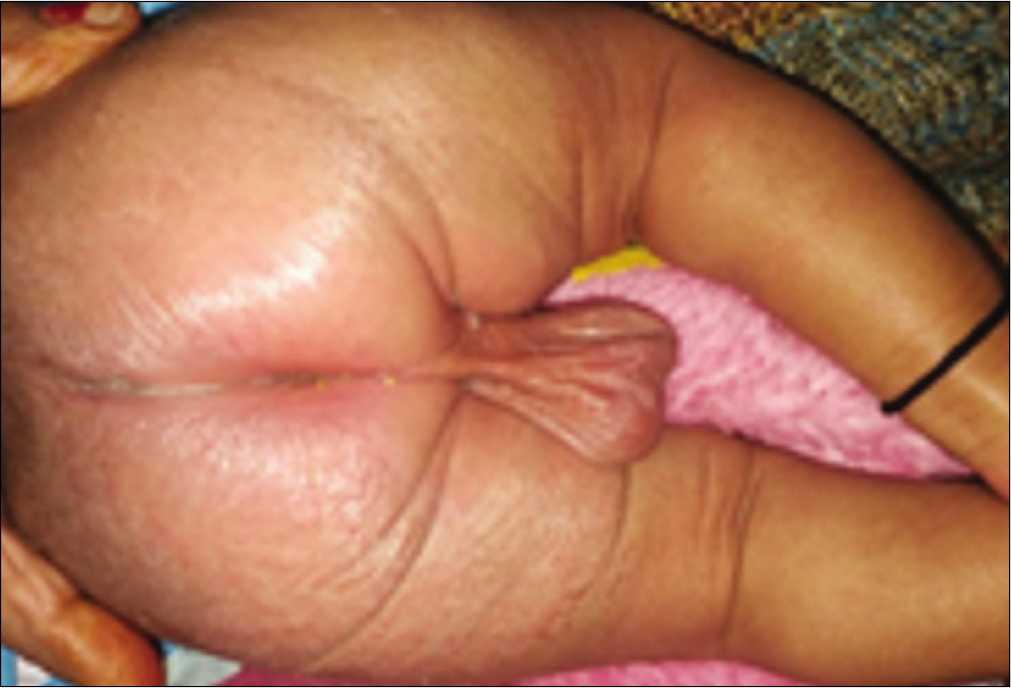
- Perineal and perianal dermatitis (background atopy helps to differentiate from wide differential diagnoses).
EYELID ECZEMA
This localized variant [Figure 8] that usually presents in spring is sometimes considered as pollinosis equivalent, with inhalant allergens playing an important role in exacerbation.[34] Constant rubbing can lead to lichenification. Allergic contact dermatitis to eye medications should be ruled out, though temporal correlation with the use of such medications and concomitant involvement of the eye give a clue. Patch testing should be able to confirm contact allergy.

- Eyelid eczema.
GENITAL ECZEMA
Vulvar dermatitis [Figure 9a] is not an uncommon cause of genital itching in atopic female patients.[31] Red and scaly plaques, often lichenified, affect the labia majora, and sometimes the labia minora too.[35] Intense itching induces rubbing and scratching, which provides temporary relief; however over time the skin thickens producing lichenification. Referred to as lichen simplex chronicus, it is an end result of the vicious itch-scratch cycle.[36] In males, penis or scrotum [Figures 9b and 9c] may be uncommonly involved.[9] In children, irritant contact dermatitis can be present concomitantly, due to poor local hygiene, friction due to tight clothing, excess moisture, and excessive soap or bubble bath use. Allergic contact dermatitis may need to be ruled out, especially in older children or adults. Regular emollients with intermittent use of topical corticosteroids or topical calcineurin inhibitors remain the mainstay of treatment. Sedative antihistamines may be required to break the itch-scratch cycle. Behavioral modification, so as to minimize rubbing or scratching can be helpful.
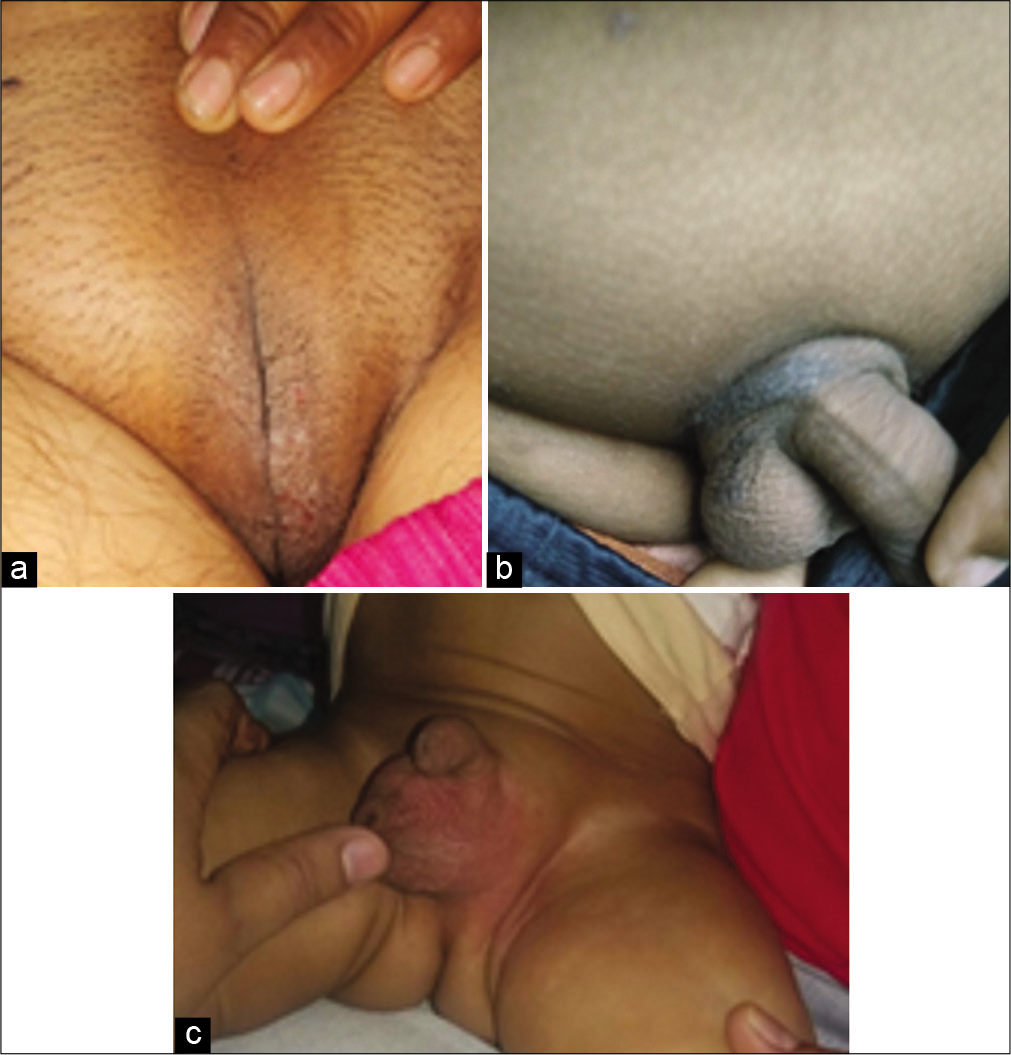
- (a) vulvar eczema (b) Genital eczema (pubic area) (c) scrotal eczema.
RETROAURICULAR ECZEMA
Intertrigo affecting the retroauricular area [Figure 10] or rhagades affecting the earlobes can be a presenting feature of atopic eczema.[9] Although seborrheic dermatitis may affect retroauricular area, examination of rest of the seborrheic sites may help in ruling out the same. Studies have shown significant association between retroauricular eczema and atopic dermatitis.[25]
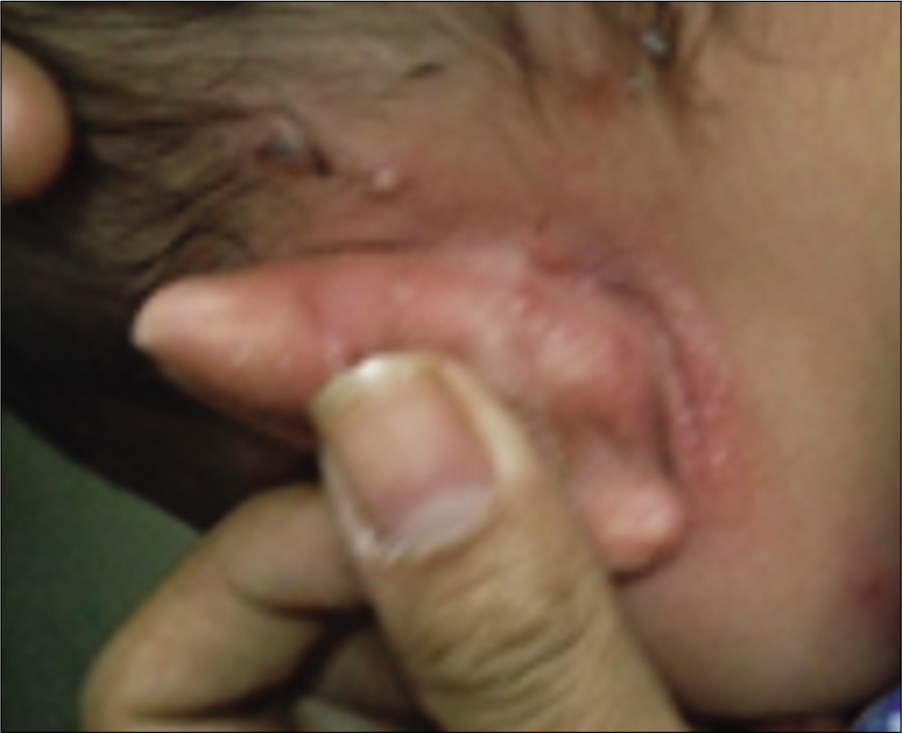
- Retroauricular eczema.
RHAGADES OF THE NASAL ORIFICES
Rhagades of the nasal orifices usually accompany chronic nasal stuffiness associated with perennial allergic rhinitis.[9]
FINGER PAD ECZEMA
Although more common in adults, adolescents or even children can present with this variant of atopic eczema [Figure 11]. Herzberg concluded that 70% of patients with finger pad eczema were women, and trauma played a major role in its development considering the fact that the first three fingers tend to get affected earlier than the last two.[37] Dominant hand involvement points to the same. Lesions are seen as erythematous scaly lesions affecting the finger pulp areas, which can subsequently develop fissuring, leading to significant impairment of hand function, and thereby the quality of life. Allergic contact dermatitis, especially with garlic or onion should be considered if first three fingers of the non-dominant hand and thumb of the other hand are affected, considering that these food items are held in the left hand while being sliced by a knife held in dominant hand.[38] Avoidance of sensitizers is of utmost importance once identified. Treatment is similar to that of hand eczema, whereby emollients remain the mainstay while topical steroids or calcineurin inhibitors are used for flares. Systemic immunosuppressants may be needed if involvement is severe enough to impair hand function and thereby impair quality of life.
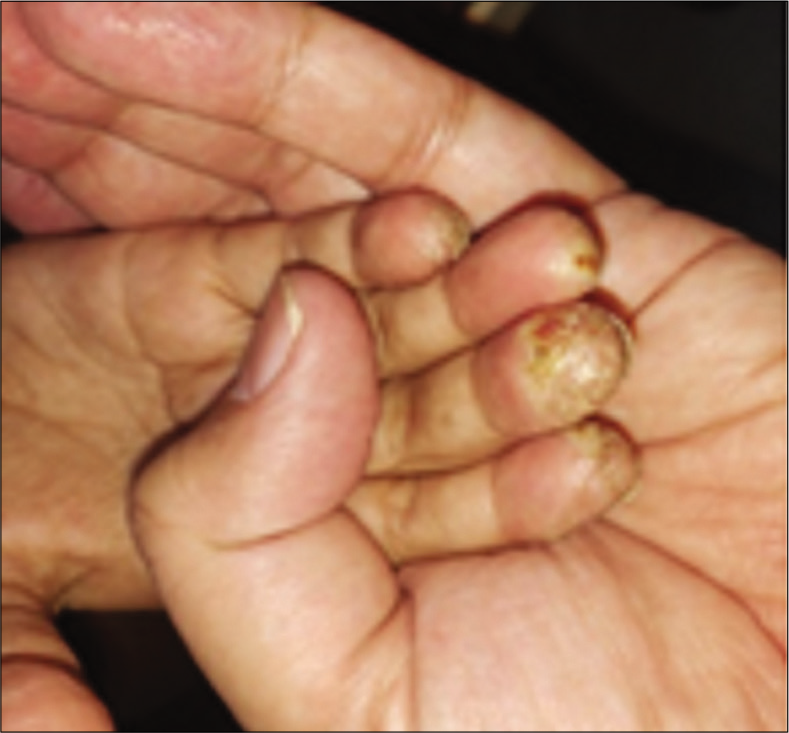
- Finger pad eczema.
ATOPIC HANDS AND FEET
Localized acral involvement is a relatively common presentation of atopic dermatitis, and is part of the minor criteria by Hanifin and Rajka.[1] Agrup in 1969 showed that one-third of the patients of atopic dermatitis had hand involvement as the initial presentation.[39] Dry scaly, itchy lesions especially on the dorsa and wrists are seen in these patients [Figure 12]. Finger pad eczema, discussed before, can either be a sole presentation or part of the more extensive hand eczema. Similar lesions on toes are referred to as atopic feet or atopic winter feet.[9] In children, these lesions tend to improve during summers or after puberty. Soaps and other irritants tend to worsen these lesions. In persistent or patterned lesions, contact dermatitis should be ruled out.[40] Avoidance of known irritants, regular use of greasier emollients and topical steroids or calcineurin inhibitors are helpful. As exposure to extraneous irritants cannot be avoided completely, periodic flares are not uncommon.
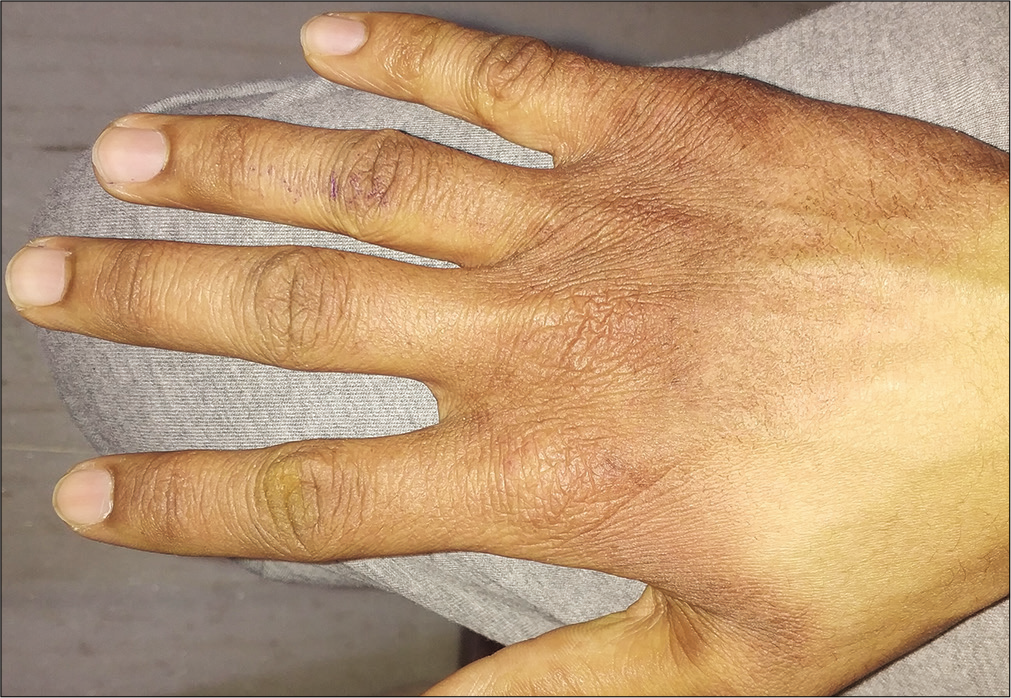
- Hand eczema in an atopic child (exacerbated by excessive soap use).
ECZEMA COXSACKIUM
Coxsackie viruses such as hand, foot, and mouth disease virus tend to show a significant flare of atopic eczema with plaques covered with vesicles and erosions [Figure 13] apart from the vesicular viral exanthem.[8,41] Referred to as eczema coxsackium, this can be an initial presentation of atopic eczema, where previously apart from the dry skin, parents had not noticed any evidence of atopy. Over recent years Coxsackie A6 has been associated with significant skin disease, mimicking varicella or drug rash, sometimes even needing hospitalization.[41] Supportive therapy is needed.
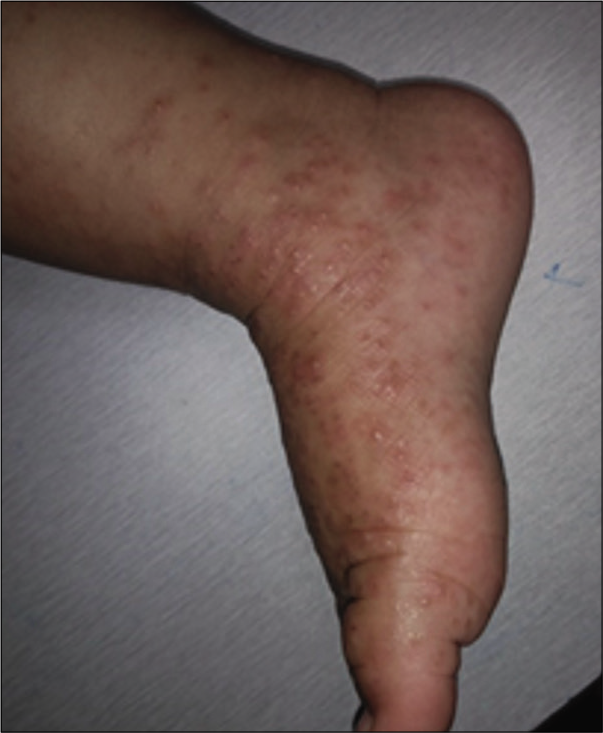
- Eczema coxsackium.
Thorough history and keen observation are needed to arrive at the diagnosis of atopic dermatitis when a patient presents with any of these atypical manifestations of the disease. Most of the times, history of pre-existing dry skin in the patient and that of some form of atopy in the family members can be elicited. Some other features that can add credence to the diagnosis of atopic eczema in these patients include palmar hyperlinearity, keratosis pilaris, Dennie-Morgan infraorbital fold, patchy facial skin including pityriasis alba, anterior dirty neck folds, intolerance to woolen or synthetic garments, and increased serum levels of immunoglobulin E. The above mentioned are part of the minor criteria by Hanifin and Rajka.[1] Although the diagnosis of atopic eczema was considered only with presence of at least three basic and three minor criteria, it is evident that many atypical presentations, though not fulfilling these to the hilt, still represent atopic eczema.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
References
- Committee of Korean atopic dermatitis association for REACH. Various diagnostic criteria for atopic dermatitis (AD): A proposal of reliable estimation of atopic dermatitis in childhood (REACH) criteria, a novel questionnaire-based diagnostic tool for AD. J Dermatol. 2016;43:376-84.
- [CrossRef] [PubMed] [Google Scholar]
- Validation of the U. K. diagnostic criteria for atopic dermatitis in a population setting. U.K. diagnostic criteria for atopic dermatitis working party. Br J Dermatol. 1996;135:12-7.
- [CrossRef] [PubMed] [Google Scholar]
- Comparative efficacy of Hanifin and Rajka's criteria and the UK working party's diagnostic criteria in diagnosis of atopic dermatitis in a hospital setting in North India. J Eur Acad Dermatol Venereol. 2006;20:853-9.
- [CrossRef] [PubMed] [Google Scholar]
- The UK working party's diagnostic criteria for atopic dermatitis; derivation of a minimum set of discriminators for atopic dermatitis. Br J Dermatol. 1994;131:383-96.
- [CrossRef] [Google Scholar]
- Prevalence of atopic dermatitis in Japanese elementary school children. Br J Dermatol. 2005;152:110-4.
- [CrossRef] [PubMed] [Google Scholar]
- Prevalence and severity of atopic dermatitis in Jeju Island: A cross-sectional study of 4, 028 Korean elementary schoolchildren by physical examination utilizing the three-item severity score. Acta Derm Venereol. 2012;92:472-4.
- [CrossRef] [PubMed] [Google Scholar]
- Typical and atypical clinical appearance of atopic dermatitis. Clin Dermatol. 2017;35:354-9.
- [CrossRef] [PubMed] [Google Scholar]
- Minimal variants of atopic eczema In: Ring J, Przybilla B, Ruzicka T, eds. Handbook of Atopic Dermatitis Vol 8. (2nd ed). Berlin: Springer-Verlag; 2006. p. :74-83.
- [CrossRef] [Google Scholar]
- Less common clinical manifestations of atopic dermatitis: Prevalence by age. Pediatr Dermatol. 2012;29:580-3.
- [CrossRef] [PubMed] [Google Scholar]
- Lichenoid and other clinical presentations of atopic dermatitis in an inner city practice. J Am Acad Dermatol. 2008;58:503-4.
- [CrossRef] [PubMed] [Google Scholar]
- Nummular dermatitis: Report of two cases in children. Arch Argent Pediatr. 2016;114:e241-4.
- [Google Scholar]
- A study of the correlation between molluscum contagiosum and atopic dermatitis in children. An Bras Dermatol. 2011;86:663-8.
- [CrossRef] [PubMed] [Google Scholar]
- Nummular eczema and contact allergy: A retrospective study. Dermatitis. 2012;23:153-7.
- [CrossRef] [PubMed] [Google Scholar]
- Relevance of patch testing in patients with nummular dermatitis. Indian J Dermatol Venereol Leprol. 2005;71:406-8.
- [CrossRef] [PubMed] [Google Scholar]
- The Asian atopic dermatitis phenotype combines features of atopic dermatitis and psoriasis with increased TH17 polarization. J Allergy Clin Immunol. 2015;136:1254-64.
- [CrossRef] [PubMed] [Google Scholar]
- Follicular eczema: A commonly misdiagnosed dermatosis. Indian Pediatr. 2012;49:599.
- [CrossRef] [PubMed] [Google Scholar]
- Eczematous Eruptions in Atlas of Pediatric Cutaneous Biodiversity Ch. 8 New York: Springer; 2004.
- [Google Scholar]
- Juvenile plantar dermatosis. Can sweat cause foot rash and peeling? Postgrad Med. 2004;115:73-5.
- [CrossRef] [PubMed] [Google Scholar]
- Sole dermatitis in children: Patch testing revisited. Pediatr Dermatol. 2012;29:254-7.
- [CrossRef] [PubMed] [Google Scholar]
- Juvenile plantar dermatosis: Wann sind epikutantestungen indiziert? Hautarzt. 1990;41:22-6.
- [Google Scholar]
- Juvenile plantar dermatosis responding to topical tacrolimus ointment. Clin Exp Dermatol. 2006;31:453-4.
- [CrossRef] [PubMed] [Google Scholar]
- Contact allergy in chronic eczematous lip dermatitis. Eur J Dermatol. 2008;18:688-92.
- [Google Scholar]
- Minor clinical features of atopic dermatitis. Evaluation of their diagnostic significance. Dermatologica. 1988;177:360-4.
- [CrossRef] [PubMed] [Google Scholar]
- Nipple eczema: A diagnostic challenge of allergic contact dermatitis. Ann Dermatol. 2014;26:413-4.
- [CrossRef] [PubMed] [Google Scholar]
- Unilateral nipple eczema in children: Report of five cases and literature review. Pediatr Dermatol. 2015;32:718-22.
- [CrossRef] [PubMed] [Google Scholar]
- Immune reactions to Pityrosporum ovale in adult patients of atopic and seborrheic dermatitis. J Am Acad Dermatol. 1990;22:739-42.
- [CrossRef] [Google Scholar]
- Risk factors and allergic manifestations associated with atopic dermatitis in Lomé (Togo): A multicenter study of 476 children aged 0-15 years. Med Sante Trop. 2016;26:88-91.
- [CrossRef] [PubMed] [Google Scholar]
- Recent microbiological shifts in perianal bacterial dermatitis: Staphylococcus aureus predominance. Pediatr Dermatol. 2009;26:696-70.
- [CrossRef] [PubMed] [Google Scholar]
- Anogenital dermatitis in patients referred for patch testing: Retrospective analysis of cross-sectional data from the North American contact dermatitis group, 1994-2004. Arch Dermatol. 2008;144:749-55.
- [CrossRef] [PubMed] [Google Scholar]
- Atopic dermatitis flare provoked by inhalant allergens. Dermatologica. 1987;178:51-3.
- [CrossRef] [PubMed] [Google Scholar]
- Wenig bekannte ausdrucksformen der neurodermitis. Arch Dermatol Forsch. 1972;244:350-2.
- [CrossRef] [PubMed] [Google Scholar]
- Substances causing contact dermatitis. Indian J Dermatol Venerol Lepr. 1978;44:264-8.
- [Google Scholar]
- Hand eczema and other hand dermatoses in South Sweden. Acta Dermatovenerol. 1969;61:29.
- [Google Scholar]
- Patch-test results in children and adolescents: Systematic review of a 15-year period. An Bras Dermatol. 2016;91:64-72.
- [CrossRef] [PubMed] [Google Scholar]
- Eczema coxsackium and unusual cutaneous findings in an Enterovirus outbreak. Pediatrics. 2013;132:e149-57.
- [CrossRef] [PubMed] [Google Scholar]






